BLOG
Contraindications You Must Know Before Laser Hair Removal
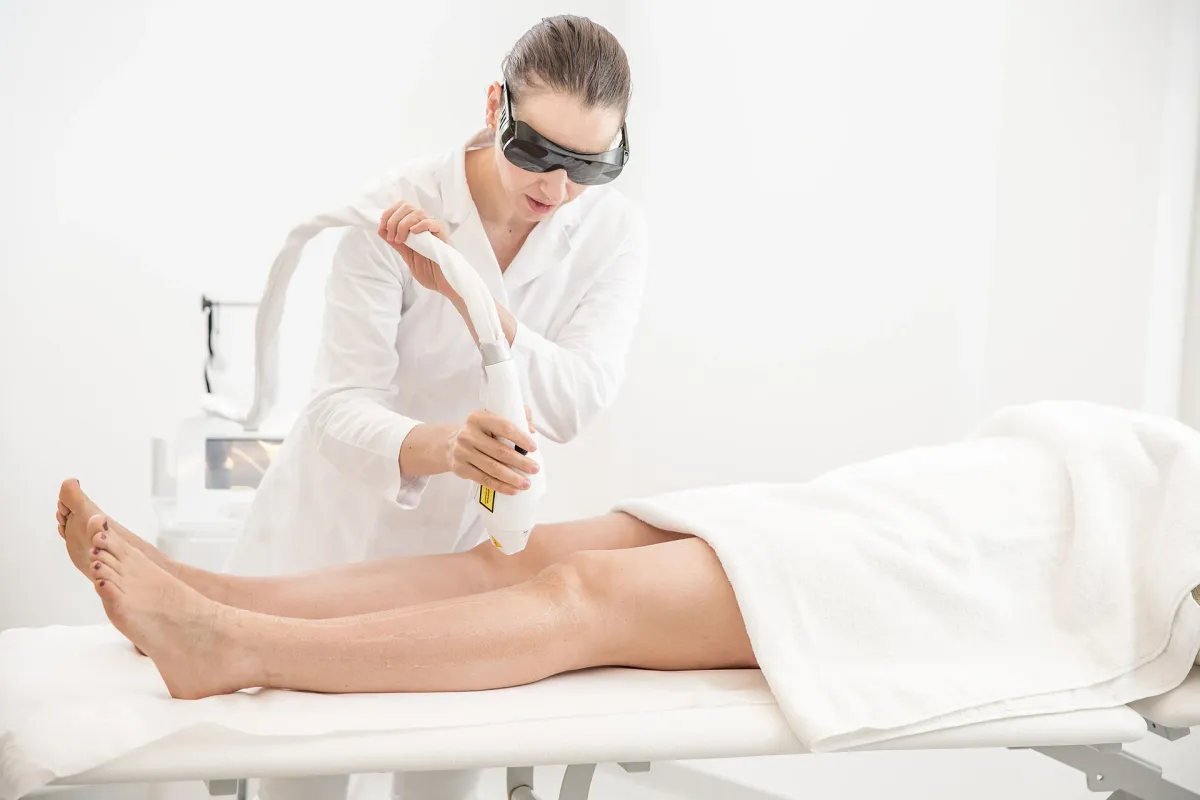
Could your health status actually worsen with laser hair removal? Find out what the studies and our experts say.
At Ethos Spa, we know undergoing any cosmetic procedure without understanding the contraindications can be nerve-wracking. What if an existing skin infection worsens? Could my lupus potentially flare up? Will those antibiotics I’m taking increase the risks?
Let our team of dermatology experts led by Dr. Hardik Soni guide you through a personalized evaluation to advise if laser hair removal is appropriate and safe based on your unique health profile.
Are There Any Laser Hair Removal Treatment Contraindications?
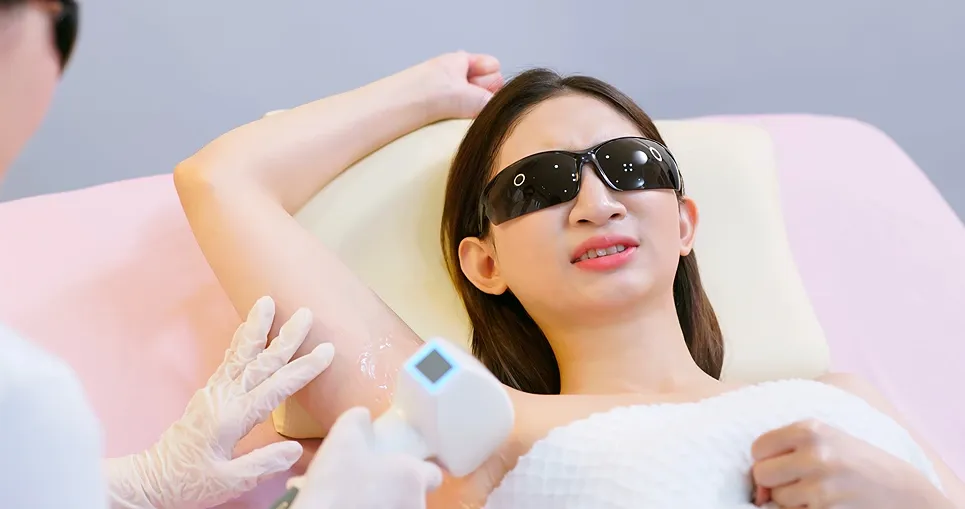
Active inflammatory skin conditions, recent sun exposure, skin lesions, photosensitizing medications, pregnancy, and keloid scarring risks may preclude laser hair removal or require precautions.
Active Inflammatory Skin Conditions
According to our experience, active flare ups of inflammatory skin disorders often represent contraindications, as laser energy can worsen conditions like acne, psoriasis, eczema, and bacterial or viral infections affecting the treatment area.
We advise waiting until any active inflammation fully resolves before considering laser therapy. Lasers can potentially trigger renewed outbreaks and inflammation when skin disorders are still on-going.
Skin Lesions and Sun Exposure
Dr. Soni also recommends avoiding laser hair removal if you have:
- Skin lesions, warts, or moles in the target region, as inadvertent stimulation of these could occur.
- Recent significant sun exposure or tanning, as lingering pigmentation and photosensitivity can increase adverse effects and risks.
Our physicians suggest waiting 1-2 months after heavy UV exposure before undergoing lasers.
Photosensitizing Medications
Certain medications like antibiotics, antifungals, and herbal supplements also warrant consideration. Why? Because they may induce photosensitivity and heighten skin sensitivity to laser light.
Dr. Soni advises stopping any potentially photosensitizing medications 1-2 weeks before treatment.
Other Precautions
Individuals prone to keloid scarring should use caution as well since even minor skin disruption carries some risk of keloid formation.
Pregnancy represents another contraindication, as the impacts of laser exposure remain unclear.
No matter your concerns or goals for silky smooth skin, our laser experts can create a customized, contraindication-free treatment plan designed with you in mind. Reach out today to learn more!
Medications Contraindicated for Laser Hair Removal
At Ethos Spa, we advise patients to inform our dermatologists about all medications they are currently taking, including prescriptions, over-the-counter drugs, herbal supplements, and vitamins.
Certain medications can potentially increase skin sensitivity and cause exaggerated responses to laser exposure.
Medications That Increase Photosensitivity
According to our clinical experience and as proven by studies, photosensitizing medications warrant caution with laser hair removal. Dr. Soni recommends avoiding treatment if you have recently taken:
- Oral isotretinoin (Accutane) for severe acne – This drug can induce prolonged photosensitivity after discontinuation.
- Photosensitizing antibiotics like doxycycline and certain antihistamines – These can heighten skin sensitivity to light.
- Some antidepressants may also increase photosensitivity and skin laser risks.
Medications That Impair Healing
Additionally, Dr. Soni advises that:
- Antineoplastic drugs used in chemotherapy warrant caution due to effects on wound healing.
- Oral corticosteroid medications may inhibit the skin’s healing abilities following laser therapy.
Chronic Conditions and Laser Hair Removal
Those with certain chronic conditions may require special considerations to maximize results and minimize risks.
Diabetes
According to our findings, diabetes poses some specific concerns with laser hair removal. Uncontrolled blood sugar can potentially lead to impaired wound healing, increased infections, scarring, and skin pigmentation changes.
However, with proper precautions like using conservative laser settings and smaller treatment areas, we can still safely perform laser hair removal for most diabetics. Frequent skin checks and optimal diabetes management are advised.
PCOS
For patients with polycystic ovarian syndrome (PCOS), laser hair removal is an excellent long-term option for treating unwanted excess hair growth.
Dr. Soni finds that with a series of 6-8 treatments, most PCOS patients will see significant hair reduction that lasts much longer compared to shaving or waxing. However, more sessions may be needed due to continual hormone fluctuations.
Hypothyroidism
Laser hair removal can be effective for those with hypothyroidism who are on medications like levothyroxine, based on our experience. As long as thyroid hormone levels are properly managed, results are often similar to those not taking the medication.
However, uncontrolled hypothyroidism can potentially lead to some hair follicle dormancy, making lasers less effective during these periods. Frequent TSH level checks are recommended.
Is Lupus a Contraindication for Laser Hair Removal?
Laser hair removal is generally not recommended for lupus patients. Non-laser alternatives like electrolysis pose less risk of triggering flares or rashes.
According to Dr. Soni, the vast majority of lupus patients experience some degree of cutaneous photosensitivity. Exposure to ultraviolet light and heat from lasers can potentially trigger flares, exacerbate rashes, and overstimulate the hyperactive immune system.
When it comes to lupus and laser safety, it’s better to be safe than sorry.
Cautious Considerations
In rare cases, a lupus patient without photosensitivity may be considered for cautious treatment under close medical supervision. However, non-laser methods like electrolysis or waxing pose far fewer risks of triggering lupus reactions.
Overall, Dr. Soni advises patients with lupus to opt for alternative hair removal options that avoid light-based devices. This minimizes the chances of stimulating the underlying autoimmune disease.
Skin Conditions as Potential Contraindications
At Ethos Spa, we carefully evaluate any skin conditions present before advising patients on the safety of laser hair removal. Certain skin disorders may require specific precautions or temporarily preclude treatment.
Acne
According to Dr. Soni, medications like isotretinoin (Accutane) and topical tretinoin (Retin-A) are contraindicated for laser hair removal due to effects on photosensitivity and wound healing. Patients taking these acne medications will need to discontinue use weeks to months prior to starting laser treatment.
Eczema
Laser hair removal is generally safe for patients with mild to moderate eczema, as long as there are no open wounds or active flare-ups in the treatment area. More severe cases may require getting the condition under control first before proceeding.
Psoriasis
Milder cases of psoriasis are typically not a contraindication. However, Dr. Soni recommends avoiding laser therapy during active flare-ups and ensuring no severe psoriatic plaques affect the treatment area. Severe widespread psoriasis may preclude lasers.
Rosacea
Rosacea does not appear to pose an inherent contraindication, according to our experience. However, as with other conditions, it is best to avoid laser hair removal during acute flare-ups to minimize risks.
Is Vitiligo a Contraindication for Laser Hair Removal?
Laser hair removal is generally not recommended for vitiligo patients, as the lack of melanin pigment poses risks of laser energy damaging depigmented skin and triggering the spread of vitiligo lesions. Non-laser alternatives are safer options.
The selective photothermolysis process used in laser hair removal relies on targeting melanin pigment within the hair follicles.
However, according to Dr. Soni, the lack of melanin in vitiliginous skin means laser energy can potentially damage these areas rather than be absorbed by the intended follicles. Multiple studies have reported cases of lasers triggering the spread of vitiligo lesions, also known as the Koebner phenomenon.
The risk seems highest with active, unstable vitiligo. Our physicians recommend thoroughly evaluating disease activity and considering all risks before proceeding with laser hair removal for vitiligo patients. In mild stable cases, cautious treatment may be possible using conservative laser settings.
But in general, Dr. Soni advises patients with extensive or active vitiligo to avoid laser procedures due to the risks of exacerbating depigmentation. Non-laser hair removal alternatives are recommended for vitiligo patients.
Waste no more time or money on temporary hair removal. Our lasers deliver unrivaled smooth skin. Experience the Ethos Spa difference today. Book now!
FAQs
Will an active herpes outbreak prevent laser hair removal?
Yes, active herpes outbreaks should be avoided before undergoing laser hair removal due to potential complications and spreading infection.
Is it advisable to have laser hair removal with an HIV or AIDS diagnosis?
No, laser hair removal is not recommended for those with HIV or AIDS as it can worsen symptoms or lead to further health complications.
Can someone with a pacemaker undergo laser hair removal?
No, laser hair removal should be avoided by those with pacemakers because the procedure can interfere with or damage the device.
How do hormonal imbalances impact laser hair removal?
Hormonal imbalances can reduce the effectiveness of laser hair removal, requiring more treatments, though it is still generally safe to undergo.
Is epilepsy considered a risk factor for laser hair removal?
Yes, epilepsy is a risk factor for laser hair removal since flashing lights can trigger seizures.
Are bleeding disorders a complication of laser hair removal?
Yes, bleeding disorders like hemophilia complicate laser hair removal due to an increased risk of bleeding and poor wound healing.
TAKE THE NEXT STEP
Begin Your Ethos Experience
Schedule your complimentary consultation and discover the Ethos difference.
book your consultation